**1. Anaphylaxis Overview:**
– Etymology: Derived from Ancient Greek terms meaning “against protection.”
– Signs and symptoms: Involves skin, respiratory, gastrointestinal, heart, vasculature, and central nervous system symptoms.
– Skin symptoms: Generalized hives, itchiness, swelling, and angioedema.
– Respiratory symptoms: Shortness of breath, wheezing, stridor, hoarseness.
– Cardiovascular symptoms: Fast heart rate, low blood pressure, shock, coronary artery spasm.
– Other symptoms: Gastrointestinal issues, confusion, headaches, anxiety.
**2. Causes and Triggers:**
– Common triggers: Venom from insect bites, foods, and medications.
– Food triggers: Common in children and young adults.
– Medication triggers: More common in older adults.
– Less common triggers: Physical factors, biological agents, food additives, and topical medications.
– Other triggers: Exercise or temperature changes.
**3. Risk Factors and Pathophysiology:**
– High-risk groups: Atopic disease sufferers, asthma patients, mastocytosis individuals.
– Pathophysiology: Rapid allergic reaction involving multiple body systems, inflammatory mediators, key cytokines, and immunologic mechanisms.
– Diagnosis: Based on signs and symptoms, criteria for anaphylaxis, and blood tests for tryptase or histamine.
– Risk factors in children: 60% with previous atopic diseases, over 90% of anaphylaxis deaths occur in those with asthma.
**4. Treatment and Management:**
– Emergency measures: Airway management, intravenous fluids, and epinephrine.
– Epinephrine: Primary treatment with intramuscular administration, repeat injections may be needed.
– Adjuncts: Antihistamines, corticosteroids, nebulized salbutamol, methylene blue, glucagon.
– Preparedness: Allergy action plan, immunotherapy, informing schools, and trigger avoidance counseling.
**5. Prognosis and References:**
– Prognosis: Good with prompt treatment, known causes, and mortality rates decreasing.
– Mortality: Occurs in 0.7-20% of cases, commonly triggered by medications.
– References: National Institute of Allergy and Infectious Diseases, research studies, guidelines, and management protocols.
Anaphylaxis is a serious, potentially fatal allergic reaction and medical emergency that is rapid in onset and requires immediate medical attention regardless of use of emergency medication on site. It typically causes more than one of the following: an itchy rash, throat closing due to swelling that can obstruct or stop breathing; severe tongue swelling that can also interfere with or stop breathing; shortness of breath, vomiting, lightheadedness, loss of consciousness, low blood pressure, and medical shock. These symptoms typically start in minutes to hours and then increase very rapidly to life-threatening levels. Urgent medical treatment is required to prevent serious harm and death, even if the patient has used an epipen or has taken other medications in response, and even if symptoms appear to be improving.
| Anaphylaxis | |
|---|---|
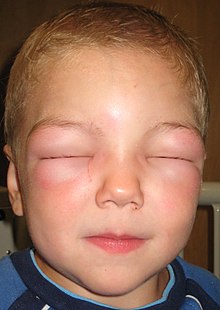 | |
| Facial angioedema in a young boy, leading to inability to open eyes. This reaction was caused by exposure to an allergen. | |
| Specialty | Allergy and immunology |
| Symptoms | Itchy rash, throat swelling, numbness, shortness of breath, lightheadedness, low blood pressure |
| Usual onset | Over minutes to hours |
| Types | Anaphylactoid reaction, anaphylactic shock, biphasic anaphylaxis |
| Causes | Insect bites, foods, medications |
| Diagnostic method | Based on symptoms |
| Differential diagnosis | Allergic reaction, angioedema, asthma exacerbation, carcinoid syndrome |
| Treatment | Epinephrine, intravenous fluids |
| Frequency | 0.05–2% |
Common causes include allergies to insect bites and stings, allergies to foods – including nuts, milk, fish, shellfish, eggs and some fresh fruits or dried fruits; allergies to sulfites – a class of food preservatives and a byproduct in some fermented foods like vinegar; allergies to medications – including some antibiotics and non-steroidal anti-inflammatory drugs (NSAIDs) like aspirin; allergy to general anaesthetic (used to make people sleep during surgery); allergy to contrast agents – dyes used in some medical tests to help certain areas of the body show up better on scans; allergy to latex – a type of rubber found in some rubber gloves and condoms. Other causes can include physical exercise, and cases may also occur in some people due to escalating reactions to simple throat irritation or may also occur without an obvious reason. The mechanism involves the release of inflammatory mediators in a rapidly escalating cascade from certain types of white blood cells triggered by either immunologic or non-immunologic mechanisms. Diagnosis is based on the presenting symptoms and signs after exposure to a potential allergen or irritant and in some cases, reaction to physical exercise.
The primary treatment of anaphylaxis is epinephrine injection into a muscle, intravenous fluids, then placing the person "in a reclining position with feet elevated to help restore normal blood flow". Additional doses of epinephrine may be required. Other measures, such as antihistamines and steroids, are complementary. Carrying an epinephrine autoinjector, commonly called an "epipen" and identification regarding the condition is recommended in people with a history of anaphylaxis. Immediately contacting ambulance / EMT services is always strongly recommended, regardless of any on site treatment. Getting to a doctor or hospital as soon as possible is absolutely required in all cases, even if it appears to be getting better.
Worldwide, 0.05–2% of the population is estimated to experience anaphylaxis at some point in life. Globally, as underreporting declined into the 2010s, the rate appeared to be increasing. It occurs most often in young people and females. About 99.7% of people hospitalized with anaphylaxis in the United States survive.
